Washington, DC (UroToday.com) As part of the SUO-CTC session on upcoming surgically relevant clinical trials in renal cell carcinoma (RCC), Dr. Ithaar Derweesh discussed the Ischemia Trial, assessing elective partial vs radical nephrectomy for tumors with increased oncologic potential. There is equipoise for this trial, as noted by Dr. Derweesh, considering that NCCN guidelines suggest that for stage II/III tumors a partial nephrectomy is reasonable if clinically indicated. The AUA guidelines have well defined (restricted) criteria for selecting patients for a radical nephrectomy, including those with an aggressive appearing tumor, no pre-existing CKD/proteinuria and a normal contralateral kidney that can provide a new baseline GFR > 45 ml/min/1.73m2.
Dr. Derweesh notes that there is always some oncologic risk with partial nephrectomy. For T1b/T2 tumors, there is a 4-5% local recurrence risk with partial nephrectomy since these are larger tumors with greater oncologic risk. A recent multi-institutional retrospective study assessed 1,250 patients who underwent partial or radical nephrectomy for clinically localized T1 renal cell carcinoma between 2006 and 2014.1 Recurrence-free survival was estimated using the Kaplan-Meier method and evaluated as a function of nephrectomy type. A total of 86 recurrences (7%) were observed during a median follow-up of 37 months. There was no difference in recurrence-free survival between partial and radical nephrectomy among all clinical stage T1 renal cell carcinomas. T3a upstaging was noted in 140 patients (11%) and recurrent disease was observed in 44 (31.4%) during a median follow-up of 38 months. Among upstaged T3a cases, partial nephrectomy was associated with shorter recurrence-free survival compared to radical nephrectomy on multivariable analysis (HR 5.39, 95% CI 1.94-14.9).
The hypothesis for the current trial is that when patients with tumors of increased oncologic risk are randomized to radical nephrectomy versus partial nephrectomy, there will be an improved recurrence free survival benefit for those undergoing radical nephrectomy. Furthermore, if partial nephrectomy is transposed to a similar higher risk population, the rate of distal recurrences in the partial nephrectomy population would go up at least 3-fold, as it would at least be similar to the radical nephrectomy population, and in reality may be worse, given the issues with suboptimal tumor control in some patients managed with partial nephrectomy. The trial schema for this trial is as follows: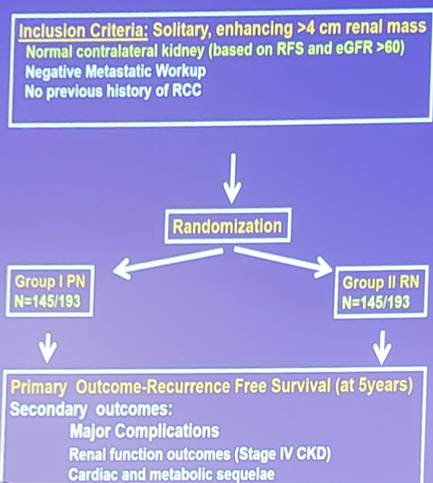
The trialists have designed this as a superiority trial given that there is a strong rationale for believing that one treatment is better than the standard of care (for cT1b/T2 RCC is partial nephrectomy whenever feasible). In patients with normal function and contralateral kidney, radical nephrectomy is a better oncologic treatment than partial nephrectomy in this setting, so it is reasonable to propose that radical nephrectomy will provide better oncologic options.
This trial has the support of ECOG, Alliance, and CCTG in Canada. It was endorsed by SWOG, but was stalled in the GU steering committee. The trial has been submitted to the SUO-CTC for support.
Presented by: Ithaar H. Derweesh, MD, Urologic Oncologist, Professor of Urology and Radiology, University of California-San Diego, San Diego, California, USA.
Written By: Zachary Klaassen, MD, MSc – Assistant Professor of Urology, Georgia Cancer Center, Augusta University/Medical College of Georgia Twitter: @zklaassen_md at the 20th Annual Meeting of the Society of Urologic Oncology (SUO), December 4 - 6, 2019, Washington, DC

